Back Pain by Daniel Zammit
Research has shown that up to 80 precent of adults will experience back pain at some time in their lives.1 What is even worse, is that many of them will experience recurring episodes.2 Lifts like the squat, deadlift, and Olympic lifts place tremendous forces on the lower back. 3 Hence, it is not a surprising that lower back injuries are among the most prevalent injuries in the population, especially in athletes.4 Finding the solution to serious back pain injuries is not an easy task, but it is definitely possible without injecting any substance, addictive non-steroidal anti-inflammatory drugs (NSAIDs) or operations.
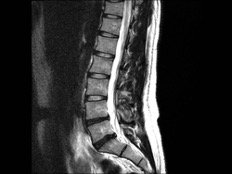 Is a picture really worth a thousand words?
Is a picture really worth a thousand words?
If a person were to take an X-Ray or MRI (Magnetic Resonance Imaging) scan, many medical doctors would presume that if something looks off on the scan, it is the exact cause of the newly developed pain the patient is feeling. However, this presumption is flawed for many reasons, including these;
- Results on imaging show poor correlation to symptoms of pain and a patient does not always know how to pinpoint the exact site of pain 5
- The MRI scan cannot show if the damage is a new “wound” or an old “scar”
- Pathology does not necessarily drive treatment
- The MRI shows only anatomy not function.
Another reason is, disc bulges are fairly common and often show up on lumbar spine MRI scans without any complaint of pain from the patient. There is enough research indicating that almost a third of healthy, pain-free 20-year-olds have a disc bulge in their spine. 6 This number increases by 10 percent for every decade of life, meaning that half of all 40-year-olds likely have a disc bulge yet are no experiencing back pain. Research has shown that just because a scan picks up an “abnormality” does not necessarily mean that it is the root cause of pain 7. Disc bulges can heal over a certain time period and no longer cause pain, even if they are still visible on an MRI scan.
It is also important to understand that an injury to the spine is different from an injury to the hip or knee. A spine injury sets off a cascade of events.8 For example, during a squat, when the spine is compressed, a healthy disc helps distribute that load evenly across the entire vertebral bone. When a disc bulge occurs, the load is no longer evenly distributed but instead is shifted to the posterior (back) aspects of the spine (facet joints). While the pain from a disc bulge may “burn out” in a few weeks or months, the mechanics of the spine are instantly changed to compensate for this bulge. How the spine carries load from then on is affected at that particular segment, and forces are shifted to the facet joints. Proper rehab that instils sufficient core stability limits the cascade of events.
Without a thorough examination, there is no way to determine if the findings from the MRI are truly the cause of pain. The evaluation process is the most crucial part in fixing back pain because it establishes the foundation on which the entire treatment plan is based.
References
- E Dreisinger and B. Nelson, Management of back pain in athletes,” Sports Medicine 21, no.4 (1996) 313-20.
- B. Andersson, “Epidemiological features of chronic low-back pain,” Lancet 354, no. 9178 (1999): 581-5.
- J. Chandler and M.H. Stone, “The squat exercise in athletic conditioning: a review of the literature,” National Strength and Conditioning Association Journal 13, no.5 (1991): 51-8
- Calhoon, Gregg, and Andrew C. Fry. “Injury rates and profiles of elite competitive weightlifters.” Journal of athletic training3 (1999): 232.
- Babińska, Anna, et al. “No association between MRI changes in the lumbar spine and intensity of pain, quality of life, depressive and anxiety symptoms in patients with low back pain.” Neurologia i neurochirurgia polska1 (2019): 74-82.
- Brinjikji, Waleed, et al. “Systematic literature review of imaging features of spinal degeneration in asymptomatic populations.” American Journal of Neuroradiology4 (2015): 811-816.
- Jensen, Maureen C., et al. “Magnetic resonance imaging of the lumbar spine in people without back pain.” New England Journal of Medicine2 (1994): 69-73.
- Singh, Kern, and Frank M. Phillips. “The biomechanics and biology of the spinal degenerative cascade.” Seminars in Spine Surgery. Vol. 17. No. 3. WB Saunders, 2005.


